Sick Sinus Syndrome
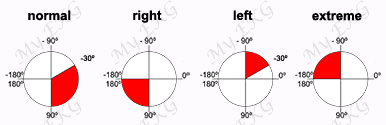
The sinus node — or Keith-Flack node — is the structure of the cardiac conduction system where the electrical impulse that triggers the heart beat is normally originated (read sinusal rhythm). It is frequently called the “natural pacemaker of the heart”.
Its morphology is fusiform and it is located in the high posterolateral wall of the right atrium, under the orifice of the superior vena cava (read cardiac conduction system).
Sick sinus syndrome (SSS) is an abnormality in the sinus node automaticity or in the stimulus conduction throughout the atria that leads to a heart rate decrease.
Sinus Pause
Sinus pause is one of the abnormalities included in the sick sinus syndrome. It is caused by the absence of electrical impulse generation in the sinus node.
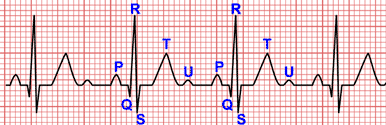
On the electrocardiogram, the main characteristic of sinus pause is the elongation of the interval between two P waves, giving the impression that a beat is missing.
Unlike sinoatrial block, previous P-P intervals in the sinus pause are regular and the P-P interval that includes the pause is less than twice the previous P-P intervals — the following P wave appears out of the regular cycle.
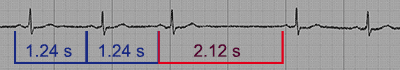
Non Pathological Sinus Pause:
Previous P-P intervals are regulars (1.24 sec), pause (red) of 2.12 sec, less than twice the previous intervals.
There is no clear consensus on when should the sinus pause be considered as pathological. Sinus pauses longer than 2 seconds in duration are frequently found on holters EKG without associated symptoms, not necessarily meaning sick sinus syndrome. Correlation of symptoms with EKG findings is important.
Generally speaking, sinus pauses longer than 3 seconds in duration are considered suggestive of sick sinus syndrome. Diagnosis should be verified with other medical analysis.
Sinoatrial Block
In sinoatrial block the sinus node generates the stimulus; however, it is not transmitted to the atria or is delayed: P waves are not generated, creating thus a pause between two P waves.
Sinoatrial block classification is similar to that of the atrioventricular blocks, but it is more difficult to diagnose.
- First degree SA block: The stimulus is delayed on its way to the atria. It can not be detected on a normal EKG.
- Second degree SA block, type I: The P-P interval progressively shortens — similar to R-R intervals in 2nd-degree AV block type I (Wenckebach phenomenon) — until a longer P-P interval appears (which contains the blocked impulse). The longest P-P interval is shorter than the sum of two consecutive intervals.
- Second degree SA block, type II: Interval without P waves which approximately equals twice the previous PP interval - although it could also be 3 or 4 times greater than the interval before the pause.
- Third degree SA block: It could be described as the absence of P waves, but it can’t be confirmed without a previous EKG tracing of the sinus rhythm or an electrophysiology study.
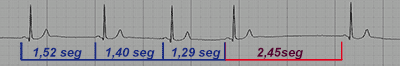
Second Degree Sinoatrial Block Type I:
The P-P interval progressively shortens until a longer P-P interval appears (red). The longest interval is shorter than the sum of two consecutive intervals.
Diferences between Second Degree Sinoatrial Block Type II and Sinus Pause
If previous P-P intervals shorten and pause duration is less than the two preceding PP intervals, diagnose is second degree sinoatrial block, type I.
If previous P-P intervals are similar and pause duration is less than the two preceding P-P intervals, diagnose is sinus pause.
If pause duration is equal to the two preceding P-P intervals, diagnose is second degree sinoatrial block, type II.
Bradycardia-Tachycardia Syndrome
Another form of sick sinus syndrome is the bradycardia-tachycardia syndrome where episodes of sinus bradycardia followed by tachyarrhythmias — mainly atrial fibrillation, but also atrial flutter or atrial tachycardia — are observed.
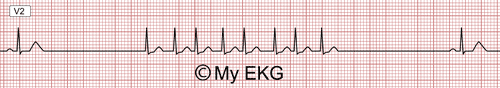
Bradycardia-Tachycardia Syndrome:
Sinus bradycardia alternating with fast atrial fibrillation ending in a long pause.
These tachyarrhythmias tend to cease spontaneously causing a long sinus pause.
Sick Sinus Syndrome and Pacemakers
Permanent pacemaker implantation is recommended for patients with relevant, documented symptomatic sinus bradycardia (heart rate below 40 bpm).
It is also recommended when symptoms cannot be associated with SSS but there is a high clinical suspicion or when there is no adequate chronotropic response to exercise performance
If you Like it... Share it.